Strabismus (Squint) often called 'crossed-eyes' or 'wall eyes'
Dr Sarda Chongtham *
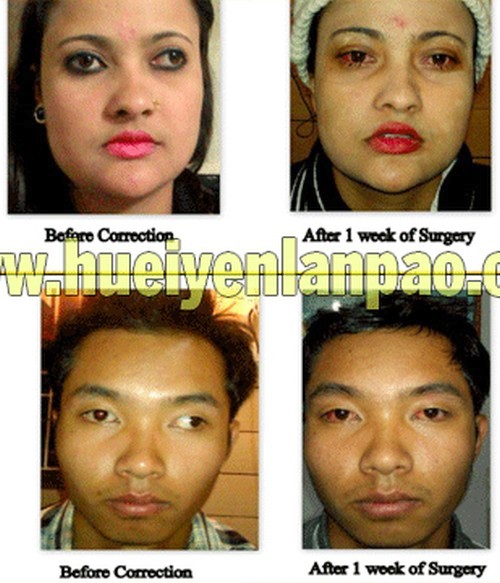
Strabismus (Squint) :: Pix - Hueiyen Lanpao
Strabismus/squint, often called "crossed-eyes" or "wall eyes' is a condition in which the eyes are not properly aligned with each other. One eye is either constantly or intermittently turned in (esotropia) or out (exotropia). This ocular misalignment may be accompanied by abnormal motility of one or both eyes, double vision, decreased vision, ocular discomfort, headaches or abnormal head posture.
Although the exact cause cannot always be determined with absolute certainty, strabismus is usually attributable to refractive, sensory or organic, anatomic or motor, or innervational causes. Young children with strabismus often develop amblyopia (lazy eye) and impaired stereopsis (binocular depth perception). The strabismic child with amblyopia has a significantly higher risk of becoming blind by losing vision in the non-amblyopic eye, due to trauma or disease. Early identification and treatment of strabismic children may prevent amblyopia.
Normal binocular vision is required for many occupational and vocational tasks, as well as many other activities in daily life. Therefore, prompt diagnosis and treatment of strabismus are critical. Symptoms such as diplopia, headaches, blurred vision, and ocular fatigue may cause individuals with intermittent strabismus who have the potential for normal binocular vision and older persons who are developing strabismus to alter their activities of daily living.
e.g., A student with intermittent strabismus may avoid reading, resulting in poor academic achievement. An employee with intermittent strabismus may suffer fatigue and headaches, resulting in reduced productivity. Strabismus may also be cosmetically displeasing and have a significant psychological impact manifested as low self-esteem, especially in patients whose jobs involve substantial personal eye contact.
Some types of strabismus, particularly those caused by high refractive errors, are preventable. Esotropias that occur due to an abnormal amount of uncorrected hyperopia are potentially preventable, if the hyperopia is diagnosed and managed prior to the onset of the deviation. More than 30 % of children with hyperopia that exceeds 4 diopters (D) develop esotropia by 3 years of age.
Whereas adult-onset strabismus can result from a neurologic disorder (e.g., brain tumor) or systemic disease (e.g., diabetes mellitus), adequate control of the general health status of a person afflicted with such a condition may lessen the possibility of the individual's developing strabismus.
Risk factors: Strabismus is more prevalent in persons with multiple handicaps, occurring in approximately 50 % of patients with Down syndrome, 44 % of patients with cerebral palsy, and 90 % of patients with craniofacial dysostosis such as Apert-Crouzon syndrome. Children born prematurely and of low birthweight have a greater risk of developing strabismus than children born at term. The prevalence of strabismus is also higher in families in which a parent or sibling has strabismus, ranging from 23 to 70 % of family members.
Age: Strabismus can develop at any age, it usually develops during childhood. Most cases begin prior to 6 years of age; the peak age of onset is around 3 years. Strabismus acquired in adolescence or adulthood is frequently either motor or sensory in origin and can be a manifestation of systemic disease (e.g., diabetes mellitus) or neurologic disorder (e.g., brain tumor). Strabismus can also develop in adults following decompensation of a heterophoria (latent strabismus). In patients of all ages, trauma to the head or orbit may result in strabismus.
Types: Misalignment of the eyes in strabismus can be classified in a number of ways:
Direction (horizontal, vertical, or cyclotorsional)
Comitant or incomitant (deviation equal in all positions of gaze or varying with the direction of gaze)
Frequency (constant or intermittent)
Involvement of accommodative system (accommodative or noaccommodative)
State of vergence system, comparing the magnitude of the distance and the near deviation (convergence-insufficiency or divergence excess exotropia; divergence-insufficiency or convergence-excess esotropia; basic esotropia or basic exotropia)
Laterality (unilateral or alternating)
Time of onset (congenital or acquired)
Size (small, moderate, or large).
Management: Ideally, preschool vision screenings should be conducted early (i.e., before 2-3 years, the peak ages for the onset of accommodative esotropia). Problems encountered in screening young children for refractive errors and strabismus may result in under detection of vision problems. Any child suspected of having strabismus should undergo a professional eye examination.
Remediation of strabismus requires treatment and management by an eye care practitioner which may include spectacle prescription, patching for amblyopia treatment and surgery, the results are usually best when instituted early.
Preservation of vision and binocular function result from proper diagnosis, treatment and management, and patient compliance. Periodic re-evaluation is very important for appropriate patient management.
* Dr Sarda Chongtham wrote this article for Hueiyen Lanpao (English Edition)
The writer is MBBS, DNB Ophthalmology (Hindu Rao, Delhi), Sir Ratan Tata Phaco Fellowship (Basic and Advanced Microsurgery), Sankara Nethralaya, Fellowship in Paediatric Ophthalmology and Adult Strabismus, Sankara Nethralaya and Consultant Ophthalmologist, Shija Eye Care Foundation
This article was posted on November 15, 2013.
* Comments posted by users in this discussion thread and other parts of this site are opinions of the individuals posting them (whose user ID is displayed alongside) and not the views of e-pao.net. We strongly recommend that users exercise responsibility, sensitivity and caution over language while writing your opinions which will be seen and read by other users. Please read a complete Guideline on using comments on this website.








