Screening for Cervical Cancer
Dr Babina Thangjam *
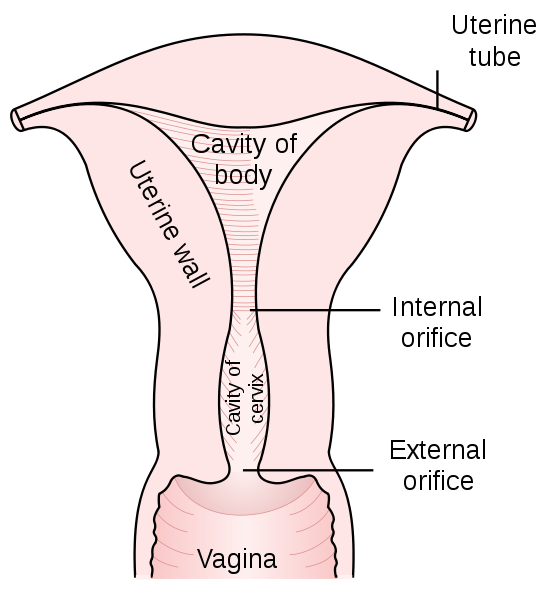
Cervix in relation to upper part of vagina and posterior portion of uterus :: Pix - Wikipedia/Mysid
When Ashangbi Devi (name changed) started having regular bouts of back pain and watery vaginal discharge, she instinctively knew something was not right. She started experiencing all thesemany years after her menopause and at first, she felt embarrassed to confide the matter to anybody. However, when the discharge became heavier and long-lasting and the back pain more intense, she finally told her daughter of her condition who immediately took her to a gynaecologist. Upon the gynaecologist's advice, Ashangbi Devi underwent a Pap smear test which revealed she had cervical cancer.
In India, one woman dies of cervical cancer every seven minutes. It has been estimated that 1.82 lakh new cases and 77,096 deaths occurred in 2010 alone which represents 29% of the global incidence and 30% of mortality. Cervical cancer is the most common cancer among women in India and continues to be the leading cause of cancer death.
Cervical cancer, or for that matter, any cancer is associated with despair and hopelessness for the patient and the family members and a diagnosis confirming cancer is received with a sense of fatalism and gloom like no other disease. It is another matter that today, Ashangbi Devi has been completely cured of the disease and is as healthy as anybody. Everybody thought she was extremely lucky because the cancer was detected in the third stage.
CERVICAL CANCER SCREENING
Despite the high mortality rates of cervical cancer, the fact remains that it is one of the most preventable forms of cancer. In India, due to lack of awareness, socio-cultural reasons, low priority of women's health issues and non-availability of early detection facilities, it is mostly detected at advanced stages when no curative treatment is possible. It has been found that 75-95% of all cervical cancer detections are at the advanced stage and this accounts for the poor survival rate in the country.
Cancer of the uterine cervix develops very slowly over 10 to 15 years following infection with the oncogenic or high-risk types of Human Papilloma Virus (HPV). The epithelial covering of the cervix initially undergoes a pre-cancerous change and at this stage, the woman usually does not have any complaints or show symptoms. This is when screening becomes significant because any delay increases the risk manifold of the pre-cancerous cellsdeveloping into cancer.
Cervical cancer screening is an essential part of a woman's routine health care. It is a way to detect pre-cancerous cervical lesions as well as early cervical cancers, both of which can be treated very successfully.In the developed countries, routine screening has been found to greatly reduce both the number of new cervical cancer diagnosed each year and deaths from the disease.The screening basically consists of cytology-based Pap smear test and HPV testing.
SCREENING BY PAP SMEAR
In a conventional Pap smear screening test, cells are collected from the surface of the cervix by a simple, painless procedure and these cells are checked for any abnormalities under the microscope by a Pathologist. If abnormal or pre-cancerous cells are found, they can be treated before they turn into cancer. In situations when cancer cells are found at an early stage, treatment becomes easy and effective.
Nowadays, automated liquid-based Pap cytology tests are used and are preferred as they reduce the number of cases of unsatisfactory or inadequate specimen and have better ability to detect cellular abnormalities. Screening tests should be advised to all asymptomatic and apparently healthy women within a target age group. Unfortunately, a Pap smear test is mostly advised when the woman is suspected to have cervical cancer either because of the symptoms or due to the unhealthy appearance of the cervix.
HPV SCREENING TEST
HPV is a very common virus, with four persons out of five having it in some stage of their lives. There are over 100 types of HPV and most women infected with HPV clear the virus naturally and do not go on to develop cervical cancer. However, a few of the HPV types have been linked to cause abnormalities of the cervical cells and in some cases, the development of cervical cancer.
Usually carried out both in enzyme-linked immunosorbent assay (ELISA) and polymerase chain reaction (PCR) methods, HPV testing is used to detect the presence of DNA or RNA from the high-risk HPV types that cause cervical cancer. These tests sometimes detect HPV infections much before abnormalities in cervical cells start appearing. HPV types 16 and 18 are believed to cause most HPV-associated cancers.HPV screening detectsthe presence of DNA from all the high-risk HPV types including HPV-16 or HPV-18.
COLPOSCOPY EXAMINATION
When cervical screening tests show evidence of abnormal cells or when several inadequate results come from these screening tests, a colposcopy examination is usually sought toexamine the area and the type of abnormality on the cervix. Colposcopy is a simple and painless procedure and can be completed within minutes.
The result shows the extent of the abnormality and indicates whether one needs further treatment or not. It has been found that a major shortcoming in the cervical cancer screening in the country is the complete absence of linkages between screening and colposcopy examination.
IDEAL AGE GROUP FOR SCREENING AND FREQUENCY
At the pre-cancer stage, women usually do not have any complaints or symptoms and it is only through screening that the disease can be detected early. Screening should be carried out on all apparently healthy women in the age group carrying greater risk, irrespective of whether they have any symptoms or not. Cervical cancer is rare before the age of 30 and, the incidence of cervical pre-cancer is considerably reduced after 60.
In India, it is recommended that screening should be carried out on all married women between the age of 30 and 60 with screening done every 5 years. A Pap smear is not a one-time test and even if the result came out normal, new changes or abnormalities can occur later after the test. One needs Pap smear testing on a regular basis, ideally, once every 3 to 5 years.
Remember, most of the time, cervical cancer cannot be seen or felt until it is advanced. This means that by the time one starts having symptoms, the cancer is already in the advanced stage and is harder to treat. Routine screening and follow-up testing are keys to prevention. Take control of your health. Make an appointment to have a screening test done today.
* Dr Babina Thangjam wrote this article for The Sangai Express
The writer is the Consultant Pathologist, BABINA Diagnostics, Imphal
This article was posted on May 30, 2013.
* Comments posted by users in this discussion thread and other parts of this site are opinions of the individuals posting them (whose user ID is displayed alongside) and not the views of e-pao.net. We strongly recommend that users exercise responsibility, sensitivity and caution over language while writing your opinions which will be seen and read by other users. Please read a complete Guideline on using comments on this website.








