Causes, diagnosis and treatment of Cirrhosis
Prof Jodhachandra Sanasam *
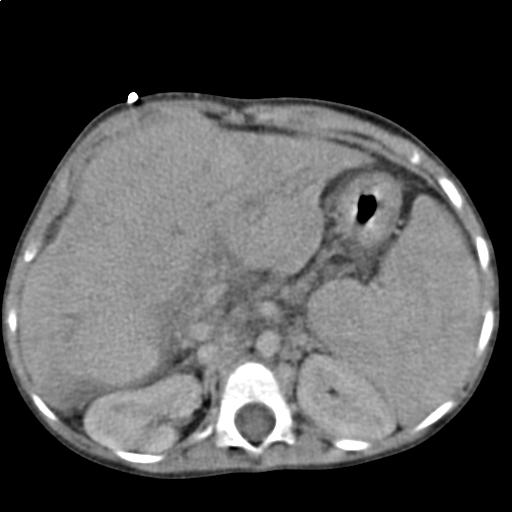
Abdominal computed tomography of a 3 year old child showing liver cirrhosis in transverse section :: Pix - Wikipedia/Christaras A
Regular heavy female drinkers are more likely to develop symptoms compared to men who consume the same amount. National Health Service (NHS) of UK postulates that excessive alcohol consumption is when a man drinks more than 3-4 units (pegs) per day and a woman drinks more than 2-4 units (pegs) per day. This does not pertain to the local brews, which contain plenty of toxic organic fatty acids.
Three most common causes of cirrhosis, if to be cited, are 'Long-term alcohol abuse', 'Hepatitis B and C infection' and 'Fatty liver disease'.
National Health Service (NHS) of UK postulates that excessive alcohol consumption is when a man drinks more than 3-4 units (pegs) per day and a woman drinks more than 2-4 units (pegs) per day. This does not
pertain to the local brews, which contain plenty of organic fatty acids, which are more toxic.
The liver breaks down toxins, including alcohol. However, if the amount of alcohol is too high, the liver weighs down under overwork and liver cells can eventually become damaged. It is not those alcoholics alone who are at risk, regular and heavy social drinking is also linked to a hihger probability of developing cirrhosis. Regular heavy female drinkers are more likely to develop symptoms compared to men who consume the same amount. The liver breaks down alcohol into carbon dioxide and water, causing fatty liver.
As soon as excessive drinking stops, the symptoms of fatty liver go away. However, 20% to 30% of those who continue drinking heavily will develop alcoholic hepatitis, the next stage. Aproximately 10% of heavy drinkers will subsequently develop cirrhosis the third stage of alcoholic liver disease.
Hepatitis and cirrhosis: Hepatitis C, a bloodborne viral infection, can damage the liver and eventually lead to cirrhosis. Hepatitis C is a common cause of cirrhosis in Western Europe, North America, and many other parts of the world including India and Manipur. Hepatitis B and D, which are less in incidence can also cause cirrhosis.
Non-alcoholic steatohepatitis (NASH), another disease that can lead to cirrhosis, is more likely to occur in people who are obese, diabetes patients, those with high blood lipid (fat) levels, as well as in individuals with high blood pressure.
Autoimmune hepatitis: When the person's own immune system attacks healthy organs, e.g. liver, then it can develop cirrhosis.
Some genetic conditions: Haemochromatosis (accumulation of iron in liver) and Wilson's disease (accumulation of copper in liver) also can cause cirrhosis.
Blockage of bile ducts: Cancer of gall bldder, bile ducts, pancreas can block the bile ducts and can cause cirrhosis.
Bud-Chiari syndrome: A disorder where thrombosis (blood clots) occurs in the liver vein can also cause cirrhosis.
Other uncommon causes: There are still some more disorders, not common; they also can cause cirrhosis.
Diagnosis of cirrhosis
A blood test particularly liver function test (LFT) is a must. The marker level of alanine transaminase (ALT) is considered to be very significant.
Imaging tests like ultrasound, CT, MRI definitely can picturise the liver for the eyes to see.
Histopathological examination of the cells, aspirated through a fine needle inserted in the liver under local anaesthesia (FNAC) can reveal the diagnosis.
Endoscopy of oesophagus and stomach may reveal presence of swollen veins, which is a hallmark sign of cirrhosis.
Treatment of cirrhosis
If diagnosed at an early stage, the damage to the liver can be restored with treatment of the underlying cause. Medications for treatment of hepatitis B or C have come up to be useful in the last few years.
Treatment for complications of cirrhosis
Ascites and oedema: Ascites (accumulation of fluid in the abdomen) or oedema (fluid retension in the legs) can be treated with a low sodium (low salt) diet and medication of diuretics to let out more urine. In severe cases, fluid may have to be drained out. Surgery is required sometimes.
Portal hypertension (Rise of pressure in the veins of intestine): Antihypertensive (blood pressure lowering) drugs can be useful. It is imperative to prevent bleeding in these veins, which can lead to further complications and death. A stent (rigid tube) in the portal vein may have to be the necessary measures.
Swollen varices (swollen veins): Vomiting of blood and or passing of bloody or black stools in a patient with bad liver are the signs of oesophageal (food pipe) varices and their rupture. Urgent procedures like endoscopic banding and sclerotherapy injection may be required. The situation may call for Sengstaken tube with balloon insertion to be retained at the junction between oesophagus and stomach, or transjugular (through the neck vein) intrahepatic portosystemic stent shunt, application of a metal tube stent across the liver to join the portal and hepatic veins.
Antibiotics for infections, quite common in bad livers, are often necessary.
IUC management is necessary for cases of hepatic coma and liver failure cases.
Liver transplant may be the only last resort when necessary if the situation is suitable.
* Prof Jodhachandra Sanasam wrote this article for Hueiyen Lanpao as part of JCB_Digs
This article was posted on April 05, 2014.
* Comments posted by users in this discussion thread and other parts of this site are opinions of the individuals posting them (whose user ID is displayed alongside) and not the views of e-pao.net. We strongly recommend that users exercise responsibility, sensitivity and caution over language while writing your opinions which will be seen and read by other users. Please read a complete Guideline on using comments on this website.








